What is PCOS - Polycystic Ovary Syndrome is a hormonal disorder that affects millions of women.2/4/2023 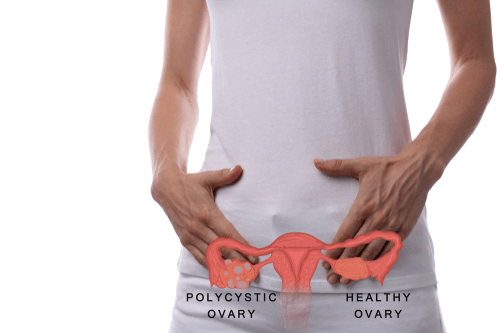 Polycystic ovary syndrome (PCOS) is a condition affecting between 1 in 10 and 1 in 20 women of childbearing age. This condition causes the body’s hormones to become unbalanced, leading to issues like ovarian cysts, increased hair growth on the face and body (hirsutism), acne, weight gain or obesity, thinning hair, irregular menstrual periods, and even infertility. It’s very likely you or someone you are close to suffers from PCOS. You must have two of the three following criteria to be diagnosed with PCOS : Irregular Periods Hyperandrogenism (Higher Testosterone) Polycystic Ovaries About 50% of people who have PCOS also suffer from obesity. Being diagnosed with PCOS is not a “death” sentence when it comes to being able to lose weight. Thankfully, more and more doctors are beginning to recognize the importance diet plays in preventing and controlling PCOS. Insulin is thought to play a major role in PCOS. This powerful hormone, released by the pancreas, exists to transport sugar out of the blood and into the cells. However, many women with PCOS are insulin resistant, meaning this process doesn’t work correctly within their bodies. As a result, high levels of insulin contribute to many of the symptoms of PCOS, such as weight gain, high cholesterol, diabetes, and ovarian cysts. Ladies, you’ll be glad to hear that controlling your diet can play a huge part in helping reverse insulin resistance. Firstly, stick to a balanced diet consisting of whole grains, fruit and vegetables, healthy fats, and protein. Losing just 5% to 10% of body weight can improve symptoms of PCOS and reduce insulin resistance. Physical activity has been shown to play an important, if not essential, role in the treatment and prevention of insulin insensitivity, meaning it’s central to the management of PCOS. At least 30 minutes of aerobic activity is recommended a week. Aim for strength training twice a week, as in order to improve insulin levels and aid weight loss, lifting weights is thought to be an important aspect of exercise for those with PCOS. Let’s have a look at the best dietary choices to decrease insulin resistance and therefore manage PCOS symptoms. While standard guidelines recommend that we get 45% to 65% of our daily calories from carbohydrates, women with PCOS should strive for the lower end of this range. If you’re already insulin resistant, a lower carb diet is typically a better option. I promise you won’t have to starve yourself to get the benefits of a lower carbohydrate intake. Even switching to a diet consisting of 43% carbohydrates has been shown to reduce fasting insulin levels, and therefore improve insulin sensitivity, in women with PCOS. Choose high fiber, whole grain carbohydrates like brown rice, oatmeal, whole rye, and whole wheat pasta in small amounts. Not only do whole grains have a lower GI rating, which improves insulin sensitivity, but they also help improve cholesterol levels – another PCOS-related complication. And don’t forget the vegetables. These are always your best source of carbohydrates, so eat plenty of them. This has to be one of my favorite topics – the importance of fats. Dietary fat is vital in a PCOS diet as it slows the release of glucose, ensuring your blood sugar levels remain relatively stable. Fat can also be important in weight management as it helps you feel full and stops overeating. One fat you can safely cut out is trans fats, which are unhealthy and now banned in the US. Trans fat raises LDL cholesterol (the bad kind), while reducing HDL cholesterol (the good kind). Since you’re already at risk of diabetes, heart disease, and high cholesterol from PCOS, you don’t need to add to the risk by eating these fats. Then you can turn to other healthy fats, namely monounsaturated and polyunsaturated fats from nuts, seeds, and avocados. No discussion on fats can leave out the importance of omega 3 fatty acids. These essential fatty acids prevent or reduce symptoms of multiple conditions, and PCOS is no exception. They don’t just decrease cholesterol and lower blood pressure, but they have also been shown to be effective in improving hirsutism and insulin resistance in patients with PCOS. The Role of Exercise Physical activity has been shown to play an important role in the treatment and prevention of insulin insensitivity, meaning it’s key to the management of PCOS. At least 30 minutes of aerobic activity is recommended a week. Aim for strength training twice a week, as in order to improve insulin levels and aid weight loss, lifting weights is thought to be an important aspect of exercise for those with PCOS. In addition to regular exercise, eating whole grain carbohydrates, healthy fats, limiting sugar, and supplementing with vitamins in order to manage your PCOS, there are a few other things to consider.
Here’s an idea of what a typical day looks like on a PCOS friendly diet – pretty good wouldn’t you say? Just make sure to adjust your portion size based on your calorie needs.
Need help on finally losing that weight for good? If you would like help on figuring out your portion sizes for your specific goals, reach out to me and apply for a free, no pressure, 15 minute coaching call. During this call we will discuss your fitness and nutrition goals and see if I can help you see that success faster. -Coach Kayli
0 Comments
Blog Post by Coach JulieNCI Certified Nutrition Coach L1 & Certified Mindset Coach I began Phase 5, the Nexium cessation phase on December 2nd. With this phase, I am moving through what was supposed to be a 4 week titration phase off of Nexium. We are currently on Week 6 of this process, which means I have definitely hit some snags and we needed to slow the process down. This is perfectly normal. Some people can complete the process in 4 weeks and others need more. Since I’ve been on this medication for 15+ years, I require some more.
During this phase, I have continued to take Zinc Carnosine at 75mg every morning on an empty stomach. I have also continued to take peppermint oil capsules before my morning and evening meals. Zinc carnosine reduces gut inflammation and helps protect the gut lining, which will be integral while my gut acid levels increase to their normal levels after being repressed for so long. Peppermint oil soothes the gut and helps prevent cramping and discomfort. I have also added DGL chewables and Betaine HCL. The DGL chewables are taken after my morning and evening meals. 3 tablets after each meal. The DGL chewable is Deglycyrrhizinated Licorice Root. I have used this supplement in a capsule form earlier in my journey. DGL is often used to soothe the stomach and support healthy digestion by encouraging mucin production. The Betaine HCL will be added in as needed, but I have not needed it yet. Betaine HCL helps protect the gut wall and strengthens it throughout the process. It will also help increase your stomach acid levels when you are struggling to recover with low stomach acid, which is common after long term use of a PPI. I will be using it as needed should I begin having acid reflux symptoms. After week one of this process, the withdrawal symptoms started. Week one consisted of reducing my Nexium to every other day rather than daily. After about day 4, I began noticing some mild diarrhea and headaches. I also noticed some weakness and dizziness. I am also having some reflux which is a most common and expected side effect. The reflux has been causing some nausea for me. Based on this, rather than moving to week 2, we decided to repeat week 1 again to see if my body would adjust. I continued to have symptoms so we decided to repeat week 1 for a third week to see if my body adjusted to the titration. My gut did regulate during the last 2 weeks of that process, so I then moved the Nexium to once every two days. I didn’t notice any reappearance of symptoms every two days, so I progressed to once every 3 days to see how my body tolerated that before we completely stopped the PepZin GI and the Nexium. After no noticeable symptoms or side effects, I took my last Nexium tablet on January 11th. Subsequently, I took my last PepZin GI tablets on January 13th. I have noticed that some meals seem to cause a slight acidic feeling in my gut. It does not feel like full heartburn or acid reflux, just a sensation that I am acutely aware of and it is manageable. One noticeable change was my bowel movements became more regular and more normal. This was something that I have not experienced in many years. Even after healing my gut I was still having a bit of constipation and this was apparent in the frequency and consistency of my bowel movements. On January 16th, I had a day of terrible heartburn. This was the first time that I have struggled with it since we started the process. The heartburn persisted for most of the week. On Tuesday, I decided to go ahead and try Betaine HCL with dinner to see if it would help. I noticed a reduction of the acidy, burning feeling shortly after taking it. The next morning I took another with my protein shake. I believe I may have taken it too soon because I felt very ill the rest of the morning. I struggled with reflux and nausea. Betaine HCL should be taken in the middle of your meal or immediately after your meal for the best effectiveness. If taken too soon or before a meal, you can get a false heartburn feeling. I took the Betaine HCL after only one drink of my protein shake and I believe this to be the cause. That same day after I ate lunch, some of the symptoms seemed to subside a little. The following day, I waited until my protein shake was complete before taking the Betaine HCL. I noticed the symptoms were greatly improved and easy to manage. It does seem that the Betaine HCL is helping increase my stomach acid levels and which is keeping the reflux to a minimum. I have noticed as the weeks progressed that my bowel movements became more regularly occurring. They also seemed to be moving toward the normal range on the Bristol Stool Scale. As always, I will provide a case study update in 4 weeks, when I should have completed this final phase if my body responds well. My body has responded exceptionally well the last few months so I am hopeful this temporary struggle will be the last and I will bounce back to normal.  Done correctly, deliberate cold exposure can positively affect brain and body health. Below, I detail some of those benefits and how best to access them. Safety Never get into a dangerous body of water. Also, never do deliberate hyperventilation before or during cold water (or any water!) immersion. Start slow (warmer than colder)—as cold shock is possible; just as with lifting weights or other forms of exercise, you’ll need to find the right temperature for you, yet prioritize safety. How cold? This is the most common question I hear, and it makes sense to ask that. However, it is truly impossible to answer, as some people tolerate cold better than others. The key is to aim for a temperature that evokes the thought, “This is really cold (!), and I want to get out, BUT I can safely stay in.” For some people, that temperature might be 60°F, whereas for others, 45°F. Here is the key: the colder the stimulus (water immersion, shower, etc.), the shorter amount of time you need to expose yourself to the cold. One study showed significant and prolonged increases in dopamine when people were in cool (60°F) water for about an hour up to their neck, with their head above water. Other studies describe significant increases in epinephrine from just 20 seconds in very cold water (~40°F). The good news is that as you do deliberate cold exposure more often, you will be more comfortable in the cold at all times and can start to use colder temperatures with more confidence, just like exercise. Ice bath, cold shower, or cryo?Most of the studies use ice baths or cold water immersion to the neck. Those are best, but cold showers can work too (and are more accessible to most). Cryo is very expensive and harder to access and not subject to much variation in protocols, so it is not considered here. To Increase Energy and Focus Deliberate cold exposure causes a significant release of epinephrine (aka adrenaline) and norepinephrine (aka noradrenaline) in the brain and body. These neurochemicals make us feel alert and can make us feel agitated and as if we need to move or vocalize during the cold exposure. Cold causes their levels to stay elevated for some time and their ongoing effect after the exposure is to increase your level of energy and focus, which can be applied to other mental and/or physical activities. Building Resilience & Grit By forcing yourself to embrace the stress of cold exposure as a meaningful self-directed challenge (i.e., stressor), you exert what is called ‘top-down control’ over deeper brain centers that regulate reflexive states. This top-down control process involves your prefrontal cortex – an area of your brain involved in planning and suppressing impulsivity. That ‘top-down’ control is the basis of what people refer to when they talk about “resilience and grit.” Importantly, it is a skill that carries over to situations outside of the deliberate cold environment, allowing you to cope better and maintain a calm, clear mind when confronted with real-world stressors. In other words, deliberate cold exposure is great training for the mind. Enhancing Your Mood While not true of every stress, cold exposure causes the prolonged release of dopamine. Dopamine is a powerful molecule capable of elevating mood, enhancing focus, attention, goal-directed behavior, etc. Even short bouts of cold exposure can cause a lasting increase in dopamine and sustained elevation of mood, energy, and focus. Metabolism In the short-term, cold exposure increases metabolism as the body has to burn calories to increase core body temperature. The total calories burned from the cold exposure are not that significant. However, the conversion of white fat (energy storage) to beige or brown fat (which are highly metabolically active) can be beneficial for:
Of course, calories on (consumed) versus calories out (metabolized) or “CICO” governs whether you gain, lose, or maintain weight. There is no escaping the laws of thermodynamics. A Solid Basic, Science-Supported Protocol Consider doing deliberate cold exposure for 11 minutes per week TOTAL. NOT per session, but rather, 2-4 sessions lasting 1-5 mins each distributed across the week. Again, the water temperature should be uncomfortably cold yet safe to stay in for a few minutes. You can do more, but this should be the minimum to achieve the benefits of cold exposure. You can do very cold, very brief exposures for adrenaline release too, but the 11 minutes is based on a recent study that explored a range of effects and is a good solid, basic protocol for ongoing use. The “Counting Walls” Approach Undoubtedly, during (or before) cold exposure, you will find your mind pushing back against the challenge. Your mind will say, “I really don’t want to do this,” even before getting in, or “Get me out of here.” You can imagine those mental barriers as ‘walls.’ Those walls are, in fact, the effects of adrenaline pulses in your brain and body, which in this case is what triggers the eventual adaptive response. After all, if it were easy, then there is no stimulus for your body to change (adapt). By maintaining top-down control of your reflexive urge to exit the cold environment, you will have successfully traversed that wall. Challenge yourself by counting walls and setting a goal of “walls” to traverse (e.g., 3-5 walls) during the round of cold exposure. You can also go for time. Up to you. The advantage of the walls approach is that it carries over to other scenarios more seamlessly, as most of life’s stressors don’t lend themselves so well to merely timing the duration until it passes. It also enhances your sense of mind-body connection to do it this way. Shivering and The Søeberg PrincipleThe Søeberg Principle based on deliberate cold researcher Dr. Susanna Søeberg is: To enhance the metabolic effects of cold, force your body to reheat on its own. Or “End With Cold.” Also, allowing your body to shiver may enhance metabolic increases from cold. Shivering causes the release of succinate from muscles and further activates brown fat thermogenesis. Try this protocol to increase shivering, either during or immediately after cold exposure: Don’t huddle or cross your arms while in the cold or after getting out. Also, don’t towel off. Let your body reheat and dry off naturally. Admittedly, this is tough. Unless doing deliberate cold exposure on a hot sunny day, admittedly, I prefer to take a hot shower and towel dry after cold exposure, but I am no doubt limiting the metabolic effect by doing that. Physical Recovery A meta-analysis of cold-water immersion effects on recovery found that cold exposure can be a highly effective recovery tool after high-intensity exercise or endurance training. Short interval (< 5 mins), cold water immersion demonstrated positive outcomes for muscle power, perceived recovery, and decreased muscle soreness (in part due to a reduction in circulating creatine kinases). The problem is that cold water immersion (but not cold showers) can limit some of the gains in hypertrophy, strength or endurance if done in the 4 hours or so after training. It’s better to wait 6 to 8 or more hours until after training, or do it before training UNLESS your goal is simply to recover without adaptation (for instance, when in a competition mode and not trying to get better, stronger, etc.) Day or night? After cold exposure, your body heats up. Yes, HEATS up. Body temperature increases tend to wake us up, whereas body temperature decreases tend to shift us toward sleepy states. Thus, I suggest using deliberate cold early in the day and not too close to bedtime. Sometimes it’s better to do it late than never, but not if it perturbs your sleep. If deliberate cold affects your sleep, try doing it earlier in the day, or not at all. Increasing the Resilience-Enhancing Effects of Deliberate Cold Exposure Staying completely still while in cold water allows a thermal layer to surround your body, ‘insulating’ you from the cold. To be most effective as a resilience training tool, move your limbs while keeping your hands and feet in the water. That will break up the thermal layer and you will experience the water as (much) colder than if you stayed still. This is also a good way to increase the potency of a cold stimulus without having to make the water colder. This is akin to slowing down the movement of a weight lift to reduce momentum and provide more tension on the working muscles. Thank you for your interest! Coach Kayli I will answer all questions! Please feel free to drop them in the comments or email me directly @ kaylimontoyafitness@gmail.com Disclaimer: KM Fitness is for general informational purposes only and does not constitute the practice of medicine, nursing or other professional health care services, including the giving of medical advice, and no doctor/patient relationship is formed. The use of information on this podcast or materials linked from this podcast is at the user’s own risk. The content of this podcast, blog and website is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Users should not disregard or delay in obtaining medical advice for any medical condition they may have and should seek the assistance of their health care professionals for any such conditions. Blog Post by Coach JulieNCI Certified Nutrition Coach L1 & Certified Mindset Coach I began Phase 4, the reintroduction phase, on July 7th. With this phase I started 2 new supplements Flora Protect and a supplement called PepZin GI. These two supplements are to repopulate the gut with good bacteria and to protect the gut barrier and gut immunity. I will maintain the S. Boulardii with these two supplements and I have continued the peppermint oil. I am reintroducing foods on a 3 day cycle. The first day, I will consume half a serving of a certain food. If I don’t have symptoms, I will continue to day two where I will consume a half serving twice per day. Assuming there are still no symptoms, I will eat a normal serving on day 3. Day 4 is a rest day, to make sure that I don’t experience any delayed symptoms. Sometimes delayed symptoms can occur if you’re experiencing constipation so we’ve built in a rest day to allow any symptoms to subside before we start a new 3 day cycle with a different food. After the end of the cycle, if there were no symptoms, I have been waiting a week or so and then reincorporating those foods back into my normal diet. Since the last update, I have reintroduced: salsa, amino energy (inulin) and alfredo. All have been a successful introduction. There were no noticeable symptoms with any of those items. Upon the completion of the 3 day cycle for these remaining foods, I had successfully completed a 21 week reintroduction phase. I did not have any foods that stood out as terrible triggers for my gut. I had some questionable issues with garlic, however I believe those to be dose dependent. This Phase ended on November 29th. I have discontinued all the supplements, including S. Boulardii, with the exception of the PepZin GI and Peppermint Oil. I will be continuing those through Phase 5, the Nexium cessation phase. We have now moved onto Phase 5, effective December 2nd. During this phase, I will move through a minimum 4 week phase where I titrate off of Nexium to discontinue its use. Long term use of a PPI (proton pump inhibitor) can be very detrimental to your health. You should be using these PPIs (Nexium, Prilosec, etc) for 3 weeks at the most to treat a temporary flare up. Long term use of PPIs can lead to increased risk of cancer, risk of fractures, pneumonia, Clostridium difficile diarrhea, hypomagnesemia, vitamin B12 deficiency, chronic kidney disease, and dementia. If you have been using these medications long term, you should not stop abruptly. You should use a step down method to gradually decrease your dose. I have been taking Nexium for over 15 years so the process will take at least 4 weeks, but could potentially last longer. During this phase, I will continue to take Zinc Carnosine at 75mg every morning on an empty stomach. I will also continue to take peppermint oil capsules before my morning and evening meals. Zinc carnosine reduces gut inflammation and helps protect the gut lining, which will be integral while my gut acid levels increase to their normal levels after being repressed for so long. Peppermint oil soothes the gut and helps prevent cramping and discomfort. I will also be adding in DGL chewables and Betaine HCL. The DGL chewables will be taken after my morning and evening meals. 3 tablets after each meal. The DGL chewable is Deglycyrrhizinated Licorice Root. I have used this supplement in a capsule form earlier in my journey. DGL is often used to soothe the stomach and support healthy digestion by encouraging mucin production. The Betaine HCL will be added in as needed. Betaine HCL helps protect the gut wall and strengthens it throughout the process. I will be using it as needed should I begin having acid reflux symptoms. After week one of this process, the withdrawal symptoms started. Week one consisted of reducing my Nexium to every other day rather than daily. After about day 4, I began noticing some mild diarrhea and headaches. I also noticed some weakness and dizziness. I am also having some reflux which is a most common and expected side effect. The reflux has been causing some nausea for me. Based on this, rather than moving to week 2, we decided to repeat week 1 again to see if my body would adjust. I continued to have symptoms so we will repeat week 1 for a third week to see if my body adjusts to the titration before moving to the next step of the process which will be reducing Nexium to once every two days. Withdrawal symptoms from a PPI are common, especially after long term use. Symptoms frequently include acid reflux and indigestion. There are, however, less common side effects that include: anxiety, depression, diarrhea, nausea, vomiting, constipation, headaches, dizziness and more. As always, I will provide a case study update in 4 weeks, when I should have completed this final phase if my body responds well. My body has responded exceptionally well the last few months so I am hopeful this trend continues. Blog Post by Coach JulieNCI Certified Nutrition Coach L1 & Certified Mindset Coach I began Phase 4, the reintroduction phase, on July 7th. With this phase I started 2 new supplements Flora Protect and a supplement called PepZin GI. These two supplements are to repopulate the gut with good bacteria and to protect the gut barrier and gut immunity. I will maintain the S. Boulardii with these two supplements and I have continued the peppermint oil. I am reintroducing foods on a 3 day cycle. The first day, I will consume half a serving of a certain food. If I don’t have symptoms, I will continue to day two where I will consume a half serving twice per day. Assuming there are still no symptoms, I will eat a normal serving on day 3. Day 4 is a rest day, to make sure that I don’t experience any delayed symptoms. Sometimes delayed symptoms can occur if you’re experiencing constipation so we’ve built in a rest day to allow any symptoms to subside before we start a new 3 day cycle with a different food. After the end of the cycle, if there were no symptoms, I have been waiting a week or so and then reincorporating those foods back into my normal diet.
Since the last update, I have reintroduced: ranch dressing, granola, avocado, ice cream, pears, beets, onion and garlic. All have been a successful introduction. The only noticeable symptoms I have had occurred during the garlic reintroduction. I had minimal stomach upset and a little bit of a bloated feeling. Not enough that I will completely exclude garlic, but I will keep it to a minimum. I am still working through a list of foods that I had eliminated and this will continue until I have tried all the foods that I eliminated so that I am either back to a normal diet or have identified some trigger foods. I am getting very close to wrapping this phase up, I have 3 more foods that I would like to add. I am taking this phase very slowly to be sure that I can clearly identify if there are some trigger foods. My coach has said that I can probably wrap it up, but I feel more comfortable maintaining this cadence until everything I used to eat is included. I have discontinued all the supplements, including S. Boulardii, with the exception of the PepZin GI and Peppermint Oil. I will be continuing those through the Nexium cessation phase. After this phase, we will move on to Phase 5 where we will eliminate Nexium and work on increasing my stomach acid levels. I have the protocol and I know what I will be adding, however I am not going to start this until I have completed the current supplementation and the reintroduction phase. With my forecasting, it looks like I will be starting that phase on December 3rd. Blog Post by Coach JulieNCI Certified Nutrition Coach L1 & Certified Mindset Coach I began Phase 4, the reintroduction phase, on July 7th. With this phase I started 2 new supplements Flora Protect and a supplement called PepZin GI. These two supplements are to repopulate the gut with good bacteria and to protect the gut barrier and gut immunity. I will maintain the S. Boulardii with these two supplements and I have continued the peppermint oil. I am reintroducing foods on a 3 day cycle. The first day, I will consume half a serving of a certain food. If I don’t have symptoms, I will continue to day two where I will consume a half serving twice per day. Assuming there are still no symptoms, I will eat a normal serving on day 3. Day 4 is a rest day, to make sure that I don’t experience any delayed symptoms. Sometimes delayed symptoms can occur if you’re experiencing constipation so we’ve built in a rest day to allow any symptoms to subside before we start a new 3 day cycle with a different food. After the end of the cycle, if there were no symptoms, I have been waiting a week or so and then reincorporating those foods back into my normal diet.
Since the last update, I have reintroduced: cauliflower, bran, kidney beans, cream cheese, honey and apples. All have been a successful introduction. I am still working through a list of foods that I had eliminated and this will continue until I have tried all the foods that I eliminated so that I am either back to a normal diet or have identified some trigger foods. I am getting very close to wrapping this phase up, I have 11 more foods that I would like to add. I am taking this phase very slowly to be sure that I can clearly identify if there are some trigger foods. My coach has said that I can probably wrap it up, but I feel more comfortable maintaining this cadence until everything I used to eat is included. I am continuing the supplement regimen that I listed above until I am out of them. When I run out, I will not be refilling those. This includes the S. Boulardii. The only supplement listed that I will continue is the peppermint oil as that will be carried over into Phase 5. After this phase, we will move on to Phase 5 where we will eliminate Nexium and work on increasing my stomach acid levels. I have the protocol and I know what I will be adding, however I am not going to start this until I have completed the current supplementation and the reintroduction phase. 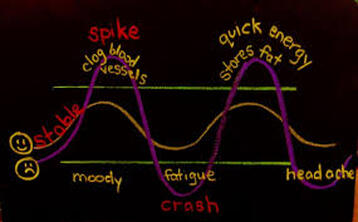 There are a few key nutrients that can make the sometimes challenging task of balancing your blood sugar easy and approachable! These three key nutrients are: fat, fiber, and protein. Other diabetes resources focus on limiting or even removing certain foods from your diet, but instead we’re going to focus on adding these three key nutrients to your plate each time you eat. . .
THE BLOOD SUGAR ROLLER COASTER
sugar and other forms of carbohydrates.
shown above.
FAT •Fat often gets a bad rep in the media and becomes feared by many, grabbing the non-fat or low-fat options at the grocery store or coffee shop. However, fat is a vital macronutrient essential in everyone's daily diet.
fat to absorb the goodness of these specific vitamins. So eating avocado or salad dressing on a salad will function both for flavor and aiding the absorption of those fat- soluble vitamins in vegetables. •Fat helps keep us full and satiated. This is simply because this macronutrient takes longer to exit the stomach, so when your meals or snacks contain fat, they help keep you satisfied longer and keep hunger away. •Fat can also slow down carbohydrate absorption, which means a more steady blood sugar response after meals and snacks.. FIBER •Fiber is great because it prevents us from getting hungry again soon after we've eaten and can help regulate blood sugar levels. •There are two types of fiber, soluble and insoluble. •Soluble fiber dissolves in water. Soluble fiber is helpful for our cholesterol and blood sugar regulation. •Insoluble fiber is not dissolvable in water and will aid in moving food through our digestive system. •A great way to increase fiber in your daily diet is to keep the skin on vegetables and fruit. So, for instance, if you're making a soup, scrub the carrots well to clean off any dirt but leave that beautiful orange skin on the vegetable to retain more fiber! PROTEIN •Protein is a macronutrient that plays a vital role in balancing our blood sugars. •Protein can be derived from animal-based sources such as meat, poultry, fish, eggs, and dairy. Protein can also be derived from plant-based sources such as whole grains, legumes, beans, nuts, and seeds. PUTTING IT INTO ACTION Toast
Dairy
Oatmeal
Rice or Pasta
- Coach Kayli Blog Post by Coach JulieNCI Certified Nutrition Coach L1 & Certified Mindset Coach I began Phase 4, the reintroduction phase, on July 7th. With this phase I started 2 new supplements Flora Protect and a supplement called PepZin GI. These two supplements are to repopulate the gut with good bacteria and to protect the gut barrier and gut immunity. I will maintain the S. Boulardii with these two supplements and I have continued the peppermint oil. I am reintroducing foods on a 3 day cycle. The first day, I will consume half a serving of a certain food. If I don’t have symptoms, I will continue to day two where I will consume a half serving twice per day. Assuming there are still no symptoms, I will eat a normal serving on day 3. Day 4 is a rest day, to make sure that I don’t experience any delayed symptoms. Sometimes delayed symptoms can occur if you’re experiencing constipation so we’ve built in a rest day to allow any symptoms to subside before we start a new 3 day cycle with a different food. After the end of the cycle, if there were no symptoms, I have been waiting a week or so and then reincorporating those foods back into my normal diet.
Since the last update, I have reintroduced: barley, cottage cheese, mayo, and peaches. All have been a successful introduction. I also took a 4 day vacation to Chicago where I ate nearly everything I wanted to without any gut upset or discomfort. I did avoid the key foods like onions and garlic that are known to be harsh offenders, but I ate foods that I haven’t consumed for years and felt totally fine. I did experience some anxiety because I was a little uncertain of how it would settle with me and being out and about and not wanting to miss out on seeing sites in town on my vacation. I am still working through a list of foods that I had eliminated and this will continue until I have tried all the foods that I eliminated so that I am either back to a normal diet or have identified some trigger foods. I am getting very close to wrapping this phase up. I am taking this phase very slowly to be sure that I can clearly identify if there are some trigger foods. After this phase, we will move on to Phase 5 where we will eliminate Nexium and work on increasing my stomach acid levels. Blog Post by Coach JulieNCI Certified Nutrition Coach L1 & Certified Mindset Coach I began Phase 4, the reintroduction phase, on July 7th. With this phase I started 2 new supplements Flora Protect and a supplement called PepZin GI. These two supplements are to repopulate the gut with good bacteria and to protect the gut barrier and gut immunity. I will maintain the S. Boulardii with these two supplements and I have continued the peppermint oil. I am reintroducing foods on a 3 day cycle. The first day, I will consume a half serving of a certain food. If I don’t have symptoms, I will continue to day two where I will consume a half serving twice per day. Assuming there are still no symptoms, I will eat a normal serving on day 3. Day 4 is a rest day, to make sure that I don’t experience any delayed symptoms. Sometimes delayed symptoms can occur if you’re experiencing constipation so we’ve built in a rest day to allow any symptoms to subside before we start a new 3 day cycle with a different food. After the end of the cycle, if there were no symptoms, I have been waiting a week or so and then reincorporating those foods back into my normal diet. So far the foods I have attempted are: watermelon, peas, hummus, gluten, Greek yogurt, ketchup, mushrooms, black beans, and raisins. So far all the foods have been tolerated except hummus. It has been hard for me to determine if the issues were actually with the hummus or issues I was having at the time with constipation causing some discomfort. I am still working through a list of foods that I had eliminated and this will continue until I have tried all the foods that I eliminated so that I am either back to a normal diet or have identified some trigger foods.
After this phase, we will move on to Phase 5 where we will eliminate Nexium and work on increasing my stomach acid levels. Blog Post by Coach JulieNCI Certified Nutrition Coach L1 & Certified Mindset Coach Throughout this process, I have continuously surprised myself. Phase 3 that I thought would last 6-12 weeks, I completed in 4. My body has been responding very well to the treatments. I have eliminated all symptoms after 4 weeks of fighting SIBO with diet and supplements. I started Phase 3 on June 3rd and ended on July 3rd. When this phase began, I was to discontinue the mastic gum and the DGL encapsulations and immediately begin the 4 SIBO supplements. The 4 new supplements were: Oregano Oil, Berberine, GI Detox and BioFilm Defense. Oregano oil is a natural antibiotic, antioxidant and anti-inflammatory. It has also been shown to help stabilize intestinal flora balance. Berberine is usually a natural alternative to some diabetes medications including metformin. Studies are showing that it has a benefit to gut microbiome and has shown to improve symptoms of diarrhea, nausea and vomiting. The BioFilm defense helps support healthy levels of biofilm and provides nutritional support for detoxing the gut. It is also an aid for bloating, gas and GI distress. Lastly, the GI Detox is exactly what it sounds like. This is a supplement that will help bind all of the harmful microbes we are trying to flush from the body and get them out of the body. I also continued the Phase 1 practices during this phase. Those steps included diet changes, starting S. Boulardii, starting colostrum, walking after meals, managing stress, getting good sleep, and keeping my workout intensity lower. These are all in place to help my body naturally detox and heal. The diet changes are to keep inflammation to a minimum. The S. Boulardii and colostrum help support the gut during the detox and die off process. Walking after meals aids with digestion and minimizes bloating and discomfort. Managing stress, getting good sleep and keep my workout intensity low are all about reserving my energy for my body’s healing and fighting the infection. It is normal to experience fatigue during this phase so keeping some energy is vital for allowing your body to recover. The typical expected symptoms associated with die off include: fatigue, muscle aches, joint pain, nausea, diarrhea, constipation, and flu like symptoms.
I did not experience any adverse symptoms during this phase. I was able to maintain consistency with the supplements and the protocol which is probably why I was able to get out of this phase within 4 weeks. Now, it’s time for Phase 4. Phase 4 is going to be continuing most of the Phase 1 protocol things. I discontinued the 4 SIBO supplements and the colostrum. I have also started taking a probiotic called Flora Protect and a supplement called PepZin GI. These two supplements are to repopulate the gut with good bacteria and to protect the gut barrier and gut immunity. I will maintain the S. Boulardii with these two supplements and I will be continuing the peppermint oil. So far the introduction of these new supplements has gone smoothly. The first day I had some cramping, but I believe this to be caused by a 3 hour window between taking the pills and eating my first meal. The supplements are to be taken on an empty stomach however I learned that my first meal needs to be shortly after I take them. The basis of this phase is reintroduction of foods. All the items that we discontinued in Phase 1 will be added back in. This is a gradual reintroduction, we aren’t just throwing caution to the wind. We are implementing a 4 day cycle. I will be choosing one food from each category and introducing it on a 4 day cycle. Day 1 will be a half a serving. If there are no symptoms, day 2 will be the same size serving twice per day. On day 3 if there are no symptoms, I will eat a normal serving. Day 4 is a rest day to allow the gut time to rest. Day 5 starts another 4 day cycle with a different food from a different food group. As we go through this process, I will be tracking what foods I’m introducing and what symptoms I experience. By the end of this, I will have identified my trigger foods, if there are any, and can avoid them to maintain gut health. I anticipate I will be in this phase until I have cycled through all the foods that I would like to add back into my diet. After this phase, we will move to Phase 5 where I work on increasing stomach acid and titrating off Nexium. Of course, you will receive an update in 4 weeks on progress. |
AuthorKayli is a certified personal trainer and online coach that specializes in fitness, wellness, nutrition, mindset, mobility and everything in between. Categories
All
Archives
April 2024
|
Call Us 620-757-9146
Home | About Us | Personal Training | Online Nutrition and Fitness Coaching | Custom Training Plans | Breakfast | Entrees | Dressings | Snacks | Blog
Phoenix Rising Podcast | Product Recommendations | Contact Me
Phoenix Rising Podcast | Product Recommendations | Contact Me
Copyright 2024 Kayli Montoya Fitness

